
Introduction
Medicaid inappropriately paid $63 million for personal care services with no record they ever occurred — a direct consequence of operating without location verification. With 4.3 million home health and personal care aides working across dispersed U.S. environments, healthcare organizations have no reliable way to verify presence, confirm compliance, or coordinate care in real time without location-aware technology.
Geofencing software addresses this directly. It creates virtual boundaries around healthcare locations — hospitals, clinics, patient homes, transport zones — that trigger automated actions when staff or patients cross them. Clock-ins become verifiable, visit logs get timestamped, and compliance trails become auditable without manual intervention. This guide breaks down the use cases, regulatory requirements, and selection criteria that matter most for healthcare operators.
TLDR:
- Geofencing automates location verification for field staff, reducing fraudulent clock-ins and supporting EVV compliance
- GPS-verified timestamps reclaim 1.5% to 5% of gross payroll lost to time theft
- HIPAA and GDPR compliance require BAAs, data minimization, and explicit consent
- Predictable, per-vehicle pricing models eliminate API cost overages as geofencing scales across large care teams
- Pilot deployments with clear KPIs prevent adoption barriers and maximize ROI
What Is Geofencing Software for Healthcare?
Geofencing software in healthcare creates virtual perimeters around specific locations—hospitals, clinics, patient homes, NEMT pickup zones—and triggers pre-configured actions when a device crosses those boundaries. Unlike retail or marketing geofencing, which targets consumers with ads, healthcare geofencing connects directly to operational systems: EHRs, CRMs, EVV platforms, and payroll. It's a compliance and workflow tool, not a marketing channel.
Core Technologies Powering Healthcare Geofencing
Four location technologies enable geofencing in healthcare settings, each suited to different environments:
| Technology | Accuracy Range | Primary Use Case | Limitations |
|---|---|---|---|
| GPS | ~4.9 meters outdoors (GPS.gov) | NEMT routing, home health EVV | Severe degradation indoors due to signal attenuation |
| Wi-Fi Fingerprinting | 10-30 meters | Hospital asset tracking, campus navigation | Vulnerable to environmental changes |
| Bluetooth Beacons | 5-10 meters | Room-level patient check-in | Requires beacon installation |
| RFID | Sub-meter | Staff badge tracking, equipment monitoring | Short range, needs dedicated readers |
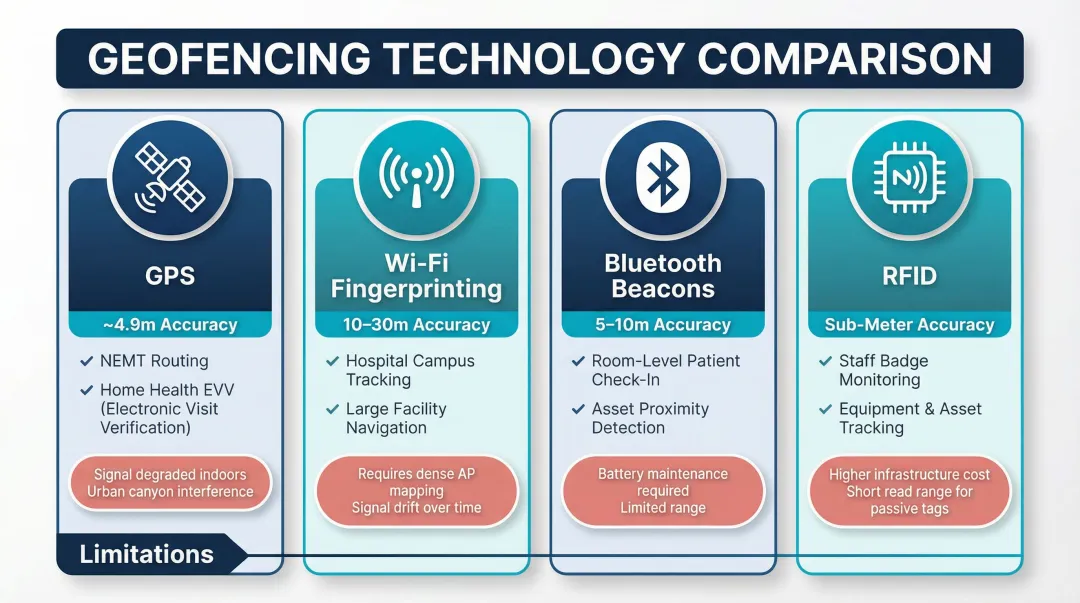
Each technology has a clear sweet spot in practice. GPS works best outdoors, covering mobile care teams traveling between patient homes or NEMT vehicles navigating city routes. Wi-Fi handles large hospital campuses where GPS signals falter, while Bluetooth beacons deliver room-level precision for patient arrival alerts. Pairing GPS with Bluetooth, for instance, lets a home health platform confirm a clinician arrived at the right address and entered the correct room.
Healthcare Geofencing vs. Generic Location Tracking
California's AB-45 law illustrates the legal distinction: geofencing healthcare facilities for targeted advertising is prohibited, but geofencing your own facility to deliver care services is explicitly permitted. Healthcare geofencing operates under different rules because it handles PHI (Protected Health Information), connects to clinical workflows, and supports federally mandated compliance programs like EVV—requirements that don't apply to retail foot-traffic analysis.
Key Healthcare Use Cases of Geofencing Software
Patient Engagement and Care Access
Geofencing enables automated patient check-in when a device crosses a facility boundary. The moment a patient arrives in the parking lot, their appointment status updates in the EHR, reducing registration queues and alerting staff to prepare. Wi-Fi or Bluetooth beacons inside the facility can then send navigation prompts: "Your appointment is in Building C, 3rd floor—turn left at the elevator."
Proximity-based patient communication sends targeted health reminders when patients are detected near a clinic they've previously visited. A diabetes clinic might trigger a screening reminder when a patient drives past the facility on their way to work. Keep messaging clinically relevant and HIPAA-compliant—patient location data carries far stricter obligations than consumer retail data.
Field Staff Verification and Home Healthcare
Home health nurses, phlebotomists, and mobile therapists use geofencing to auto-log visit arrival and departure at patient addresses. When a caregiver's device enters a pre-defined geofence around a patient's home, the system timestamps the event and creates a verifiable proof-of-service record. This eliminates self-reported timesheets and removes disputes over whether a visit occurred.
Preventing buddy punching and fraudulent clock-ins becomes automatic. If an employee clocks in from a coffee shop 10 miles from the patient's address, the system flags the anomaly instantly. Operations managers gain real-time visibility: Is the 2 p.m. visit happening on time and at the correct location? Geofencing answers this without phone calls.
NEMT and Medical Transportation
Non-Emergency Medical Transportation (NEMT) providers manage approximately 200 million trips annually in the U.S. Geofencing creates zones around pickup points, hospitals, and drop-off locations so dispatchers receive automated alerts when vehicles enter or exit each stop. This supports on-time performance tracking and eliminates manual check-in calls from drivers.
For NEMT and paratransit fleets, this requires an API that handles multi-stop, real-time location intelligence at volume. NextBillion.ai's Geofencing API lets fleets define custom radius zones, trigger webhooks for entry/exit events, and feed location data directly into dispatch and billing systems—at predictable per-vehicle pricing rather than per-API-call rates that scale poorly for high-frequency healthcare trips.
Behavioral Health and EVV Compliance
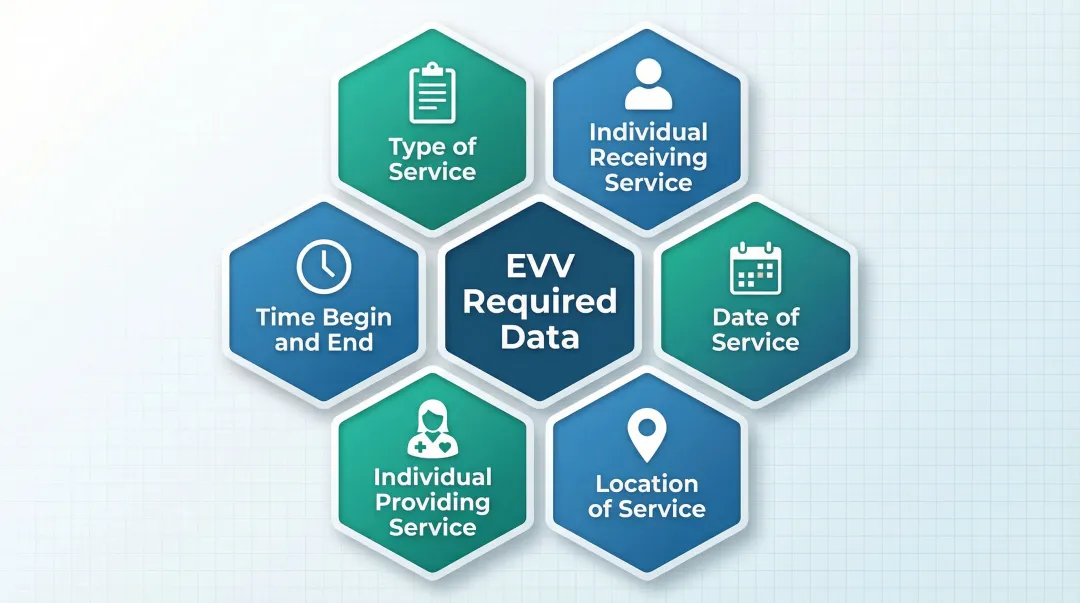
The 21st Century Cures Act (42 U.S.C. § 1396b(l)) mandates Electronic Visit Verification (EVV) for Medicaid-funded personal care and home health services. The law requires capturing six data elements at each visit:
- Type of service performed
- Individual receiving the service
- Date of the service
- Location of service delivery
- Individual providing the service
- Time the service begins and ends
Behavioral health practices—ABA therapy centers, home-based counseling—must verify caregiver physical presence at each visit. Geofencing automates this by capturing GPS-verified check-in/check-out timestamps, creating a location-verified audit trail that reduces fraudulent billing risk and protects against penalty exposure. CMS guidance confirms GPS isn't strictly required (IVR is a permitted alternative), but geofencing is the most scalable, automated path to compliance.
Benefits of Geofencing Software for Healthcare Organizations
Operational Efficiency Through Automation
Location-triggered workflows eliminate manual administrative steps. When a therapist arrives at a client site, the system automatically logs the visit, updates the schedule, sends notifications to supervisors, and queues the billing entry—all without human intervention. Operations teams scale field staff coverage without adding administrative headcount.
Accurate Payroll and Reduced Time Fraud
The American Payroll Association estimates that time theft costs employers 1.5% to 5% of gross payroll annually. GPS-verified clock-in/out timestamps replace self-reported hours, automatically flagging early departures and off-site entries. Organizations see measurable reductions in timesheet corrections and payroll overpayments within the first billing cycle.
Improved Patient Safety and Care Continuity
Geofencing ensures the right caregiver is at the right location for the right shift duration. When a home health aide's device never enters the patient's geofence during a scheduled visit, the system alerts supervisors immediately. This reduces no-shows and shift gaps that directly impact patient outcomes.
Real-Time Visibility and Proactive Management
Managers receive instant alerts when anomalies occur:
- Staff clocking in outside approved zones
- Therapists overdue at client sites
- NEMT vehicles delayed at pickup locations
Teams intervene before staffing gaps escalate into patient safety incidents or compliance violations.
Compliance and Accountability Through Verifiable Records
Location-stamped audit trails support accreditation reviews, regulatory audits, and dispute resolution. For organizations billing Medicaid or Medicare—where one state projected $5 million in first-year EVV savings due to reduced inappropriate payments—documentation rigor isn't optional. Every geofenced visit creates a verifiable, timestamped record tied to a specific location.

Privacy, Compliance, and HIPAA Considerations
HIPAA (United States)
Geographic location data qualifies as Protected Health Information (PHI) when tied to healthcare interactions. HHS OCR guidance specifies that geographic subdivisions smaller than a state—including street addresses, cities, and ZIP codes—must be treated as PHI. Healthcare organizations must ensure any geofencing vendor signs a Business Associate Agreement (BAA).
Key HIPAA requirements for geofencing:
- Data minimization: Capture location only at clock-in/out events, not continuously
- Purpose limitation: Use location data solely for visit verification, not secondary marketing
- Retention limits: Delete location records after audit periods expire
- Clear policies: Document what is tracked, why, and for how long
HHS OCR guidance on tracking technologies clarifies that if a vendor creates, receives, or transmits PHI, a BAA is mandatory.
GDPR (European Union/United Kingdom)
Under GDPR, location data is personal data that requires a lawful basis for processing—either explicit consent or legitimate interest (Article 6). Healthcare organizations operating in the EU or UK must:
- Obtain explicit consent from tracked employees and patients
- Inform users what data is collected, by whom, and for what purpose
- Honor the right to erasure (deletion requests)
- Minimize data collection to what's strictly necessary
State-Level and Sector-Specific Rules
Several U.S. states impose additional restrictions beyond HIPAA. Key rules to know:
- New York Civil Rights Law § 52-c: Requires written notice upon hiring for any employee monitoring program
- Illinois BIPA: Demands explicit consent for biometric data collection; courts in some states extend this to include precise location tracking
- EVV mandate (21st Century Cures Act): A separate federal requirement—distinct from HIPAA—that specifically targets home health and behavioral health providers, mandating electronic visit verification for Medicaid-reimbursed services
Best Practices for Privacy-Respecting Implementation
- Event-based, not continuous tracking: Capture location only when devices cross geofence boundaries
- Role-based access controls: Limit who can view location data to supervisors with legitimate operational need
- Explicit written consent: Obtain consent from all tracked employees and patients before deployment
- Clear opt-out mechanisms: Provide employees with transparent opt-out procedures where legally permissible
- Regular audits: Review data retention policies and access logs quarterly

How to Choose the Right Geofencing Software for Healthcare
Key Capability Checklist
Evaluate vendors on these must-have features:
- HIPAA/BAA compliance: Vendor willingness to sign comprehensive BAA
- EVV integration: Direct connectors to EVV platforms and payroll systems
- Offline mode: Functionality in rural or low-connectivity settings where field staff operate
- Customizable geofence radius: Ability to set zones from 50 meters to 5 kilometers
- Real-time alerts: Instant notifications for entry/exit events and anomalies
- HIS/EHR/CRM integration: Open APIs or pre-built connectors to existing systems
- API availability: For healthcare tech companies building geofencing into proprietary platforms
For healthcare technology companies embedding geofencing into their own software, the checklist above points toward one specific requirement: an API-first architecture. NextBillion.ai is built for this use case — its geofencing infrastructure supports custom configurations, predictable per-vehicle pricing, and deployment at scale without the per-API-call costs that make traditional mapping providers expensive at volume.
Deployment and Scalability Considerations
Two deployment paths dominate healthcare geofencing:
| Approach | Best For | Key Strengths |
|---|---|---|
| Out-of-the-box workforce tools | Direct care providers needing fast EVV compliance | Preconfigured integrations, simple setup, field-ready mobile apps |
| API/SDK-based platforms | Enterprises and health tech companies embedding geofencing into proprietary systems | Custom location triggers, webhook control, EHR/CRM/payroll integration |
Evaluating Accuracy and Reliability
Test geofence accuracy in both indoor and outdoor environments. GPS drift in large hospital buildings is a known challenge—signals bounce off walls, creating multipath errors. Ask vendors:
- What fallback verification methods exist? (Wi-Fi, Bluetooth)
- How does the system handle low-connectivity rural areas?
- What uptime SLAs are offered for patient-safety-critical workflows?
Request pilot deployments in your actual operating environments—not just vendor demos. Monitor false positives (staff flagged as off-site when legitimately at a location) and false negatives (missed check-ins) over at least two weeks before committing.
Implementation Best Practices
Phase the Rollout
Start with a small pilot team in a single region or facility. Monitor for false positives, collect staff feedback on battery drain and app usability, and refine geofence boundaries before organization-wide deployment. A 50-person pilot over 4-6 weeks reveals edge cases that won't surface in controlled testing.
Engage Staff Transparently
Employee resistance is the most common adoption barrier. Communicate the purpose and limitations of geofencing clearly:
- "This system verifies you were at Mrs. Johnson's home at 2 p.m., but it doesn't track your route or monitor you continuously."
- Lead with what staff gain: "No more disputed timesheets. No more manual visit logs."
- Obtain written consent and address privacy concerns directly in all-hands meetings.
Once staff are aligned, turn attention to the metrics that will tell you whether the rollout is actually working.
Define KPIs Before Launch and Monitor Continuously
Set measurable targets before go-live:
- Reduction in timesheet edits (target: 40% decrease in first quarter)
- EVV compliance rate (target: 98% documented visits)
- On-time visit completion (target: 85% within 15-minute window)
Review location-data reports against these benchmarks over a 6-to-8-month window. When targets aren't met, the data itself points to the cause — either geofence accuracy (a technical fix) or staff not carrying devices (a training and policy fix).
Frequently Asked Questions
What is geofencing in healthcare?
Geofencing in healthcare uses virtual location boundaries—built with GPS, Wi-Fi, or Bluetooth—around facilities or patient locations to trigger automated actions such as staff check-ins, patient notifications, or compliance logs when a device enters or exits the zone.
Is geofencing in healthcare HIPAA compliant?
Geofencing can be HIPAA compliant when implemented correctly. Key requirements include a signed BAA with the vendor, treating location data as PHI, limiting collection to entry/exit events rather than continuous tracking, and maintaining clear consent and data retention policies.
How does geofencing support Electronic Visit Verification (EVV)?
EVV mandates require proof of caregiver location, visit time, and duration for Medicaid-funded services. Geofencing automates this by capturing GPS-verified check-in/check-out timestamps that satisfy federal and state EVV requirements.
What is the difference between GPS, Wi-Fi, and Bluetooth geofencing in healthcare?
Each technology serves a different range and environment:
- GPS — best for outdoor and vehicle tracking (~5–10 meter accuracy)
- Wi-Fi — suited for large hospital campuses (10–30 meters)
- Bluetooth beacons — room-level precision indoors (5–10 meters)
The strongest implementations combine all three.
Can geofencing software integrate with existing EHR and CRM systems?
Most modern geofencing platforms connect with HIS, EHR, CRM, and payroll systems through open APIs or built-in connectors. This lets location-triggered workflows feed directly into existing records, eliminating manual data entry.
Does geofencing track employees continuously or only at check-in/check-out?
Most healthcare geofencing platforms capture location only when a device crosses a boundary (enter/exit event), not continuously. This limits data collection, reduces battery drain, and keeps the solution aligned with HIPAA and GDPR privacy principles.


